Scientists at the University of Cambridge have discovered a new mechanism that may prevent the spread of brain cancer cells. By regulating key molecules in the extracellular matrix, they can alter the growth environment of glioblastoma. This discovery could open new avenues for treating this highly invasive and frequently recurring type of brain cancer.
Glioblastoma is the most common malignant brain tumor, with a five-year survival rate of approximately 15%. Current treatments include surgical resection, radiotherapy, and drug interventions, but their effectiveness is often limited by cancer cell invasion and postoperative recurrence. A research team from the Yusuf Hamied Department of Chemistry at the University of Cambridge proposes that instead of directly targeting cancer cells, modifying the surrounding extracellular matrix may effectively inhibit tumor invasion.
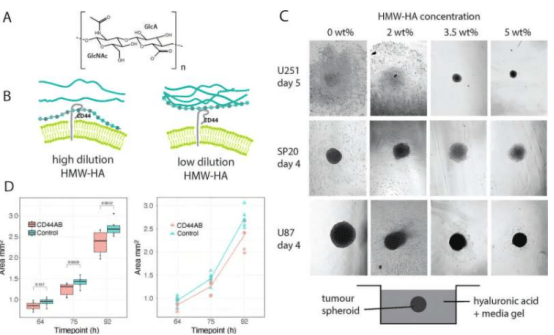
The researchers found that cancer cells rely on the binding of hyaluronic acid (HA) in the extracellular matrix to the surface receptor CD44 to gain the ability to migrate and invade. By using cross-linking technology to immobilize hyaluronic acid molecules, their flexibility can be restricted, thereby blocking the signaling with the receptor. Professor Melinda Duer, who led the study, stated: "Hyaluronic acid needs to maintain a certain degree of flexibility to interact with cancer cells. If we can restrict this flexibility, we can prevent cancer cells from spreading. This approach does not kill the cells but changes their behavior."
The research was published in the journal Royal Society Open Science. The team used techniques such as nuclear magnetic resonance spectroscopy to verify this mechanism. Even under low concentrations of hyaluronic acid, immobilizing the molecular structure could still significantly suppress cancer cell activity, indicating that the effect is not due to physical blockage but rather biological signal reprogramming.
This strategy also helps explain why glioblastoma often recurs in the surgical area. Postoperative local edema may dilute hyaluronic acid, increasing its flexibility and thereby promoting the invasion of residual cancer cells. Stabilizing the matrix environment may help reduce the risk of postoperative recurrence.
Professor Duer added: "Modifying the microenvironment in which cancer cells reside offers a new possibility for regulating the progression of various solid tumors. This method does not rely on drugs penetrating every cell and holds good application potential." The team's next step is to further validate this strategy in animal models to lay the foundation for future clinical trials.
